Choosing the right alcohol recovery program is not about finding the “best rehab.” It is about finding the best fit for your health, your risks, your schedule, and your support needs. When the fit is right, you stay longer, learn more, and relapse less often.
What does “right alcohol recovery program” mean for your situation?
Start with three questions:
- Safety: Do you need medical support to stop drinking safely?
- Structure: How much daily support do you need to stay on track?
- Support: Do you need help with mental health, stress, trauma, or family issues?
Good programs match care to the person, not the other way around. The ASAM Criteria is a widely used framework that places people based on medical, psychological, and social needs, not on willpower.
Do you need medical detox or withdrawal management first?
Some people can stop drinking with outpatient care. Others need supervised withdrawal care. Withdrawal can be dangerous after heavy or long-term drinking.
Ask a clinician right away if you have any of these:
- past withdrawal seizures
- hallucinations or confusion during past quit attempts
- very heavy daily drinking
- serious heart, liver, or seizure conditions
- mixed substance use
- pregnancy
If you are unsure, get a medical check. Safety comes first.
What level of care fits your needs: outpatient, IOP, residential, or inpatient?
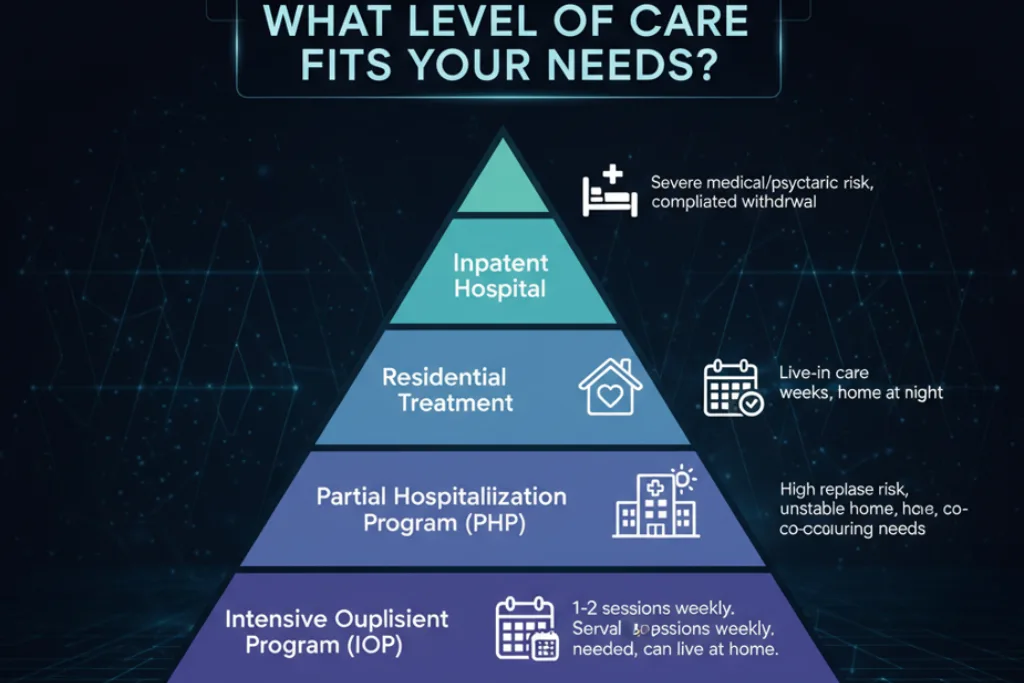
Programs are often grouped by level of care. Higher levels mean more time, more staff, and more structure.
Common options
- Outpatient therapy: 1–2 sessions weekly. Best for mild to moderate cases, stable home, strong support.
- Intensive outpatient program (IOP): several sessions weekly. Best when you need structure but can live at home.
- Partial hospitalization program (PHP): daytime treatment most days, home at night.
- Residential treatment: live-in care for weeks. Best for high relapse risk, unstable home, or serious co-occurring needs.
- Inpatient hospital care: for severe medical or psychiatric risk, or complicated withdrawal.
A quality provider will assess you across health, mental health, daily life, and relapse risk before recommending a level of care.
What evidence-based treatments should the program offer?
Look for programs that offer a menu of proven options, not one single method. NIAAA notes that evidence-based care often includes behavioral treatments, FDA-approved medications, mutual-support groups, or a mix.
Therapies to ask about
- CBT (Cognitive Behavioral Therapy): builds coping skills, changes drinking thoughts and habits.
- Motivational approaches: helps you strengthen your reasons for change.
- Relapse prevention planning: triggers, cravings, high-risk events, “what to do next” steps.
- Family or couples support (when helpful): improves home support and reduces conflict.
If a program cannot clearly explain what methods they use and why, keep looking.
Should you choose abstinence-based care or a moderation goal?
Some programs require total abstinence. Others support reduction goals. Your best choice depends on:
- history of control loss
- health risks
- prior relapse pattern
- personal safety and life stability
If alcohol has caused repeated harm, strong cravings, or failed “cut down” attempts, abstinence-focused care is often safer. If you are unsure, choose a program that can discuss goals without shame and can adjust the plan based on your progress.
Should the program include medication support for alcohol cravings?
Many people never hear about medications for alcohol use disorder, even though they can help. NIAAA lists FDA-approved medications as part of evidence-based care.
Common FDA-approved options include:
- naltrexone
- acamprosate
- disulfiram
What matters is not which medication is “best online.” What matters is whether the program can:
- screen your health risks
- explain options in plain language
- monitor side effects
- combine medication with therapy and support
If a facility discourages medication without medical reasons, that is a red flag.
Do you need “dual diagnosis” care for mental health and trauma?
Alcohol use often overlaps with:
- anxiety
- depression
- trauma symptoms
- sleep problems
If mental health symptoms are present, you need a program that can treat both at the same time. Many people relapse when stress, panic, or low mood stays untreated.
Ask directly:
- “Do you treat anxiety and depression on-site?”
- “Do you have licensed mental health clinicians?”
- “How do you handle trauma care safely?”
Can telehealth or online programs work for alcohol recovery?

Yes, for many people. Telehealth can reduce barriers like travel, schedule limits, and stigma. SAMHSA provides guidance on using telehealth for substance use treatment.
Digital care is also improving. A randomized clinical trial in JAMA Network Open found support for a digital CBT program with brief clinical monitoring for adults seeking treatment for alcohol use.
Telehealth works best when you have:
- a safe home environment
- stable internet access
- no severe withdrawal risk
- a plan for emergencies and cravings
If your home is chaotic or unsafe, in-person structure may be better.
How do you check if a program is high quality and safe?
Use this quality checklist.
Staff and licensing
- licensed addiction counselors or therapists
- medical staff available when needed
- clear supervision and clinical leadership
Accreditation and standards
Accreditation does not guarantee perfection, but it can signal outside review. The Joint Commission accredits many behavioral health organizations, including addiction treatment.
Clear treatment planning
- full assessment at intake
- written plan with goals you understand
- progress checks and plan updates
Aftercare planning
- relapse plan
- follow-up schedule
- step-down care options (IOP → outpatient)
- peer support connections
Transparency
- clear pricing
- insurance details in writing
- no pressure tactics
What red flags should make you walk away?
Avoid programs that:
- promise a “100% cure”
- refuse to explain methods
- use only confrontation or shame
- do not screen for withdrawal risk
- block family contact without clinical reason
- push you into a level of care without assessment
- hide costs or add surprise fees
- discourage outside medical care
A good program earns trust through clarity, not pressure.
What questions should you ask before enrolling?
Bring these questions to every call.
Fit and level of care
- “What level of care do you recommend, and why?”
- “What happens if I relapse during care?”
Treatment approach
- “What therapies do you use most?”
- “How do you teach craving and trigger skills?”
Medical support
- “Do you screen for withdrawal risk?”
- “Do you offer medication options for alcohol cravings?”
Mental health
- “Do you treat anxiety, depression, or trauma here?”
- “Can I keep my current mental health meds?”
Family and work
- “Can family be involved if I want that?”
- “Do you offer evening or weekend sessions?”
Outcomes and aftercare
- “What does aftercare look like for the next 90 days?”
- “Do you help me step down to a lower level of care?”
How do you compare programs side by side without getting overwhelmed?
Make a simple scorecard. Rate each item 0–2.
- matches your safety needs
- level of care makes sense
- evidence-based therapy offered
- medication support available when appropriate
- mental health care available if needed
- schedule fits your life
- aftercare plan is clear
- costs are clear
- staff credentials are clear
- you feel respected on the call
Choose the alcohol recovery program with the highest score, not the fanciest website.
Where can you find reliable treatment directories and referral help?

If you are in the United States, SAMHSA offers:
- a 24/7 helpline for treatment referral and information
- FindTreatment.gov for a confidential locator
If you are outside the U.S., use the same approach:
- start with hospital systems, medical colleges, or government health services
- ask about licensing and credentials
- confirm withdrawal safety planning
- confirm evidence-based methods
Conclusion: What is the simplest way to choose the right program?
Pick a program the same way you would pick care for any serious health condition:
- Start with safety (withdrawal risk, medical needs).
- Match the level of care to your relapse risk and daily support needs.
- Choose evidence-based care that includes therapy, recovery supports, and medication options when appropriate.
- Demand a clear aftercare plan for the next 90 days.
- Avoid red flags and pressure tactics.
Recovery works better when the plan fits your real life and your real risks.
Clear Mind Sobriety – Want help choosing a program without confusion or sales pressure? Clear Mind Sobriety offers personalized support, practical tools, and virtual guidance to help you pick the right level of care and build a plan you can follow.





